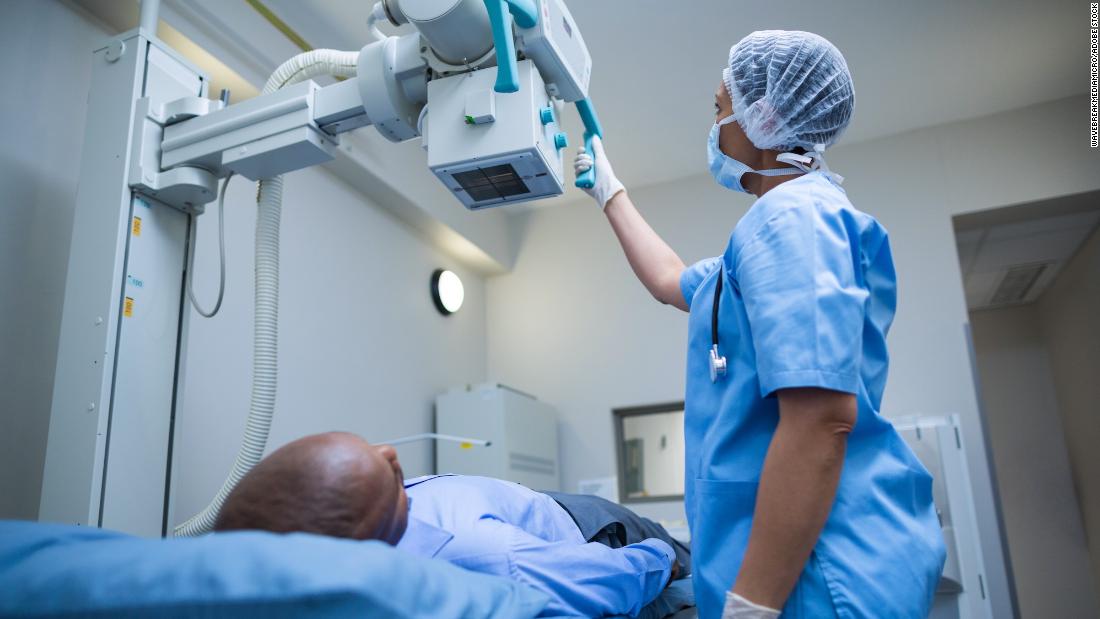
Early research suggests promising use of AI to predict risk of heart attack or stroke using a single chest X-ray
The face of heart attacks is changing in the US
01:00 – Source: CNN
CNN —
Early research suggests a promising use of artificial intelligence to predict the 10-year risk of death from a heart attack or stroke from a single chest X-ray.
The preliminary findings were presented Tuesday at the annual meeting of the Radiological Society of North America. The research is in the final draft stages and has not been submitted for publication in a medical journal.
Researchers used nearly 150,000 chest X-rays to train an artificial intelligence program to identify patterns in the images associated with risk from major cardiovascular disease events. They tested the program on a separate group of about 11,000 people and found “significant association” between the risk level predicted by the AI and the actual occurrence of a major cardiovascular disease event.
The clinical standard for analyzing risk from cardiovascular disease is the atherosclerotic cardiovascular disease (ASCVD) risk score, a calculator that weights various patient data points that have been found to have a high association with adverse cardiovascular events, including age, blood pressure and history of smoking.
Statin medication is recommended for people with a 10-year risk of 7.5% or higher. The AI model uses the same risk thresholds as the established risk calculator, and early findings suggest that it works just as well.
“We’ve long recognized that X-rays capture information beyond traditional diagnostic findings, but we haven’t used this data because we haven’t had robust, reliable methods,” said Dr. Jakob Weiss, the lead researcher and a radiologist affiliated with Massachusetts General Hospital and the AI in Medicine program at Harvard Medical School’s Brigham and Women’s Hospital.
Sometimes, the AI findings align with a traditional radiology reading, but other times, it picks up on things that may have been missed, he said.
“Part of it is anatomical alterations that we would also pick up with our naked eye and that make physiological sense. Let’s say there’s increased blood pressure or cardiac failure – these are findings that we can pick up in a normal chest radiograph as well. But I think a lot of the information captured or extracted is somewhere embedded in the scan, but we can’t make sense of it as traditionally trained radiologists as of now,” Weiss said.
“It has this black box character to it,” he said, which can sometimes make it hard to communicate risk to patients without an explanation to pinpoint.
Dr. Donald Lloyd-Jones, chair of preventive medicine at Northwestern University’s Feinberg School of Medicine and former president of the American Heart Association, was co-chair of the risk assessment panel when the ASCVD risk calculator was created in 2013 and a key player in 2018 when the guidelines were updated to emphasize the relationship between the risk score and personal medical history.
He was not involved in the new AI research but says it’s important to keep the field moving forward.
“This is exactly the kind of application that artificial intelligence is best for,” he said. “So we need to continue to do things like this to really understand if we can find, particularly, patients who would otherwise slip through the cracks. I think that’s where it may be most useful.”
But collecting all of the patient data points that go into the established risk calculator is still critical – because they’re actionable. And whether risk is calculated using a statistical formula or an AI model, the most successful outcomes will still require personalized patient assessments.
“We don’t cure smoking by a chest X-ray. We actually need to work with the patient to find ways to get them to stop smoking,” Lloyd-Jones said. “The risk calculator is one part of risk assessment, but it’s not the only part. It’s a process that involves both the patient and the doctor in a discussion about what is the patient’s risk and how much we think a statin would help them.”
For their research, Weiss and co-authors trained the AI using chest X-rays from participants in the National Cancer Institute’s Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial. It was tested on people who had a routine outpatient chest X-ray at Mass General Brigham and were potentially eligible for statin therapy, with an average age of 60.
Additional research, including a controlled randomized trial, is necessary to validate the deep learning model.
Source: https://www.cnn.com/2022/11/29/health/heart-attack-stroke-x-ray/index.html