Three Vaccinated U.S. Senators Test Positive for Virus


Senators Roger Wicker, Republican of Mississippi, Angus King, independent of Maine, and John Hickenlooper, Democrat of Denver, said on Thursday that they had tested positive for the coronavirus, adding to the number of breakthrough cases among lawmakers.
“Senator Wicker is fully vaccinated against Covid-19, is in good health and is being treated by his Tupelo-based physician,” his spokesman, Phillip Waller, said in a statement released by his office, adding that the senator was experiencing only mild symptoms.
The announcement from Mr. Wicker came as his home state has shattered previous records for new cases this week, and is now reporting more new cases relative to its population than any other state in the country. Mississippi is averaging 118 new cases a day for every 100,000 people, according to data compiled by The New York Times.
Mr. King’s statement said he was symptomatic but taking recommended precautions.
“While I am not feeling great, I’m definitely feeling much better than I would have without the vaccine,” he said. “I am taking this diagnosis very seriously, quarantining myself at home and telling the few people I’ve been in contact with to get tested in order to limit any further spread.”
Mr. Hickenlooper said on Twitter that he was experiencing limited symptoms and expressed gratitude to scientists who had developed the vaccine. He also encouraged vaccinated people to get booster shots in accordance with a plan that the Centers for Disease Control and Prevention announced this week.
The Senate is in recess this week after adjourning early last Wednesday, leaving it unclear whether any of the men had been in recent contact with other lawmakers, as well as when or where they were first exposed. Their diagnoses brings to 11 the number of senators who have tested positive so far, according to news reports compiled by Ballotpedia, a political data website; more than 50 members of the House have tested positive.
Several other vaccinated politicians have recently announced breakthrough cases of their own, including Senator Lindsey Graham of South Carolina, who said he tested positive for the virus after attending a gathering hosted by Senator Joe Manchin III of West Virginia.
On Tuesday, Gov. Greg Abbott of Texas tested positive and began receiving an antibody treatment, highlighting both the growing concerns over breakthrough cases in the United States and the political tensions over public health measures that Mr. Abbott has consistently opposed in his home state.
While Mr. Wicker has encouraged his constituents to get vaccinated and has applauded the national vaccination effort in official statements, he has also resisted elements of the Biden administration’s coronavirus response. In June, he introduced a resolution calling on the C.D.C. to end a mask mandate for vaccinated people on public transportation.
As the Delta variant spreads aggressively, infections in vaccinated people have been seen more frequently, though they are still rare. The surge and the rising frequency of breakthrough infections have prompted agencies to extend public health measures. The Transportation Security Administration said on Tuesday that the mask mandate would remain in effect on public transportation through Jan. 18.

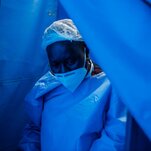
NAIROBI, Kenya — The Africa director at the World Health Organization, Dr. Matshidiso Moeti, criticized the decisions by some wealthy nations to start administering coronavirus booster shots, saying the decisions “make a mockery of vaccine equity” when the African continent is still struggling to get vaccine supplies.
African countries continue to lag far behind other continents in inoculations, with only 2 percent of the continent’s 1.3 billion people fully vaccinated against Covid-19 so far. Though vaccine shipments have accelerated in recent weeks, African nations are still not getting nearly enough to meet their needs, Dr. Moeti said.
Instead of offering additional doses to their already fully vaccinated citizens, she said, rich countries should give priority to poor nations, some of which are being ravaged by the coronavirus pandemic.
“Moves by some countries globally to introduce booster shots threaten the promise of a brighter tomorrow for Africa,” Dr. Moeti said in an online news conference on Thursday. “As some richer countries hoard vaccines, they make a mockery of vaccine equity.”
The World Health Organization has called for a moratorium on booster shots until the end of September to free up vaccine supplies for low-income nations. But several wealthy nations have said they would not wait that long. In the United States, the Biden administration said on Wednesday that it would provide booster shots to most Americans beginning as soon as Sept. 20. France and Germany also said they plan to offer shots to vulnerable populations, and Israel has already given third shots to more than a million residents.
President Biden said in a television interview broadcast on Thursday that he and his wife, Jill Biden, plan to get booster shots themselves, assuming federal regulators give the go-ahead.
Mr. Biden defended offering Americans an additional shot when many countries were struggling to deliver initial doses to their populations.
“We’re providing more to the rest of the world than all the rest of the world combined,” Mr. Biden said in the interview on ABC. “We’re keeping our part of the bargain.”
Africa has so far reported more than 7.3 million cases and 184,000 deaths from the coronavirus, according to the W.H.O. The virus is now surging in about two dozen African nations, pushing many governments to impose lockdowns, extend overnight curfews, close schools and limit public gatherings.
Health experts say the more contagious Delta variant, first detected in India, is responsible for most of the current spread on the continent. “While it took eight months for Alpha to spread to 30 countries, Delta has done so in half that time — only four months,” Dr. Moeti said, comparing Delta to a variant first detected in Britain.
Several African countries are also dealing with outbreaks of other diseases. This week, Ivory Coast confirmed its first Ebola case in almost 30 years. Guinea reported a case of the Marburg virus, the first ever found in West Africa. Uganda, which just emerged from a 42-day coronavirus lockdown, announced a polio outbreak.
Dr. Moeti urged wealthy nations to “rethink the idea of boosters” because of the danger that more dangerous variants will arise as the virus spreads in unvaccinated populations.
“Failure to vaccinate the most at-risk groups in all countries will result in needless deaths,” she said. “We say this every week, and it cannot be repeated enough.”
Michael D. Shear contributed reporting.

New York’s digital vaccine app, the Excelsior Pass, will likely cost far more than originally expected, with projected costs nearing $27 million, according to newly obtained documents shared with The New York Times.
The pass is stepping into the spotlight this week as restaurants, museums, gyms and other indoor venues in New York City are asking customers — often for the first time — to show proof of at least one vaccine dose as part of a new city mandate.
More than three million people have already retrieved an Excelsior Pass, which consists of a QR code that can be stored on a smartphone or printed out, the state said. The app verifies applications against city and state vaccination records, and the code is generated only once someone is considered fully vaccinated, defined as at least 14 days after the final shot.
Through a Freedom of Information Request, the Surveillance Technology Oversight Project, an advocacy group that has expressed concern about the privacy and security implications of vaccine passports, received the latest contract between the state and I.B.M., which is developing the app.
In June, the advocacy group provided The Times with the original version of the contract between the state and I.B.M., which estimated the total cost of the project would be $17 million over three years. Even that was far more than the $2.5 million in development costs that Mr. Cuomo and his staff had publicly mentioned when announcing the arrival of the nation’s first government-sponsored digital app that verifies proof of vaccination.
The updated version of the contract, signed by the state’s Office of Information Technology Services in late June, adds another $10 million. New York, the contract states, had already incurred an extra $656,421 in charges for technical support and updates. And a Phase 2 of the project, which was mentioned but not described in detail in the original contract, ended up costing more than double than estimated, rising to $4.7 million from $2.2 million.
“We always said that Excelsior Pass would be a high-tech distraction from real public health measures, but we had no idea the price would go up this high,” said Albert Fox Cahn, the executive director of the Surveillance Technology Oversight Project. “Even as New Yorkers find themselves on the hook for millions more, the app still isn’t able to do a lot of the basics.”
The governor’s office did not immediately return a request for comment about the contract.
The contract lists some of the issues that software engineers were called in to fix, such as incorrect error messages and crashes. Engineers added foreign language capability, access for the visually impaired and, to address a common problem, made it so the phone number entered by a user does not need to match what is listed in the vaccine registries. The fixes are ongoing. Not until June, the contract indicates, did the app make it possible for someone who has periods in their name (like T.J.) to retrieve a pass.
Some users are still having trouble finding their passes, sometimes because the registries have outdated information listed, like an old ZIP code. In order to find a person’s vaccination record, the app checks his or her name, date of birth, ZIP code and county of vaccination against the vaccine registry, and nearly all information must match. Some 4 percent of users who tried to get passes in the app’s opening months were unable to, the state said.
Phase 2 of the contract included the development of what the state has called Excelsior Pass Plus, which launched on Aug. 4. The main enhancement of the Plus pass is that it now includes the date, place and type of vaccination in the QR code, instead of just verifying that a person is vaccinated. That information will be shared when the app is scanned, but it allows for a wider range of places to use it as vaccination proof.
American Airlines is accepting the pass for travel to some international destinations. Both the original and the Plus pass also allow users to show results of P.C.R. and antigen tests, the state said.
For now, the Excelsior Pass is available for New Yorkers vaccinated in state, and New Yorkers vaccinated out of state who ask their health care providers to upload that information to the New York vaccine registries. But that may be about to change.
The contract also lays out a new, previously undisclosed Phase 3, which is projected to cost $6.7 million. By this summer, the contract states, the app was expected to begin including data from New Jersey and Vermont, which presumably means more people vaccinated in those states would be able to get passes. And the app is scheduled to add the ability to track third doses, just in time for booster shots, assuming federal regulators authorize them.

Covid precautions have turned many parts of our world into a giant salad bar, with plastic barriers separating sales clerks from shoppers, dividing customers at nail salons and shielding students from their classmates.
Intuition tells us a plastic shield would be protective against germs. But scientists who study aerosols, air flow and ventilation say that much of the time, the barriers don’t help and probably give people a false sense of security. And sometimes the barriers can make things worse.
Research suggests that in some instances, a barrier protecting a clerk behind a checkout counter may redirect the germs to another worker or customer. Rows of clear plastic shields, like those you might find in a nail salon or classroom, can also impede normal air flow and ventilation.
Under normal conditions in stores, classrooms and offices, exhaled breath particles disperse, carried by air currents and, depending on the ventilation system, are replaced by fresh air roughly every 15 to 30 minutes. But erecting plastic barriers can change air flow in a room, disrupt normal ventilation and create “dead zones,” where viral aerosol particles can build up and become highly concentrated.
“If you have a forest of barriers in a classroom, it’s going to interfere with proper ventilation of that room,” said Linsey Marr, professor of civil and environmental engineering at Virginia Tech and one of the world’s leading experts on viral transmission. “Everybody’s aerosols are going to be trapped and stuck there and building up, and they will end up spreading beyond your own desk.”

Florida’s state board of education threatened this week to penalize local school board members and superintendents in Broward and Alachua Counties because they were requiring students to wear masks at school.
But those threats did not stop Florida’s largest school district, Miami-Dade, as well as the school districts in Hillsborough County, which includes Tampa, and Palm Beach County, from approving similarly strict mask mandates on Wednesday, in further defiance of the state board.
“Yesterday, I spoke with a mother of a child who died,” Alberto Carvalho, the superintendent of the Miami-Dade County Public Schools, told the state board of education on Wednesday. “Over the week, I’ve spoken with employees and their relatives, begging me to do the right thing.”
He said he would “wear proudly as a badge of honor” any consequences that may come from his recommendation to require masks, which the school board adopted with a 7-1 vote later on Wednesday.
Lubby Navarro, a board member, cast the lone dissenting vote. “I am not going to sit here and violate state law,” she said.
Battles over school mask policies have engulfed Florida as hospitals have filled with Covid-19 patients, many of them young people. In Broward County, local officials warned this week that only five beds remained available in pediatric intensive care units there.
This month, Gov. Ron DeSantis, a Republican, ordered school districts to allow parents to opt out of mask requirements for their children. He also allowed parents whose children feel “bullied” by mask mandates to apply for a private-school voucher.
The Hillsborough County Public Schools began the school year on Aug. 10 with parents allowed to opt out of its mask requirement. But the district quickly found so much virus in its schools that the board called a special meeting on Wednesday to consider stricter rules. They voted 5-2 to limit mask opt-outs to students with medical exemptions, in spite of a recommendation from Addison G. Davis, the superintendent, that the district keep its existing rules.
“Right now, I think it’s really important to mask our children,” said Nadia T. Combs, one of the board members. She added that she’s “not here for the adults.”
“I’m not here for politics,” she said. “I’m here to keep kids in school.”
In the last week, the district has had to quarantine or isolate 10,384 out of its more than 214,000 students — nearly 5 percent — because of virus exposure.
The emotional meeting in Tampa on Wednesday featured masked parents — some of them health care workers wearing scrubs — pleading for a stronger mandate, and unmasked parents — some of them wearing “Freedom Fighter” T-shirts — insisting on keeping the existing rules.
“My children need to be unmasked,” said Kelly Boynton, one of the opponents. “It’s tyranny.”
Before the meeting, Jennifer Buschner, who has two children in the district, said that her daughter, who is in second grade and has a rare genetic disorder, had hoped to return to the classroom, but the lack of a mask mandate made it too dangerous.
“I was appalled,” Ms. Buschner said. “They took my daughter’s safety away from her, and made it so that she has to be home.”
The county school boards in Alachua (based in Gainesville) and Broward (in Fort Lauderdale) each voted to require masks, with allowances for medical exemptions signed by a physician or other health care provider. The districts argued that such a mandate complied with both state health regulations and the governor’s order.
But the state board of education disagreed. On Tuesday, the board directed the state commissioner of education to investigate and punish the two districts by withholding funds, suspending or removing school board members, or withholding their salaries.
Video
transcript
transcript
Biden Announces Virus Measures for Schools and Nursing Homes
The Biden administration said that it would take steps to protect educators from reprisals in states whose governors have banned mask requirements and that it would leverage federal funding to force nursing home staff to be vaccinated against the coronavirus.
-
Some politicians are trying to turn public safety measures, that is, children wearing masks in school and the political disputes, for their own political gain. Some are even trying to take power away from local educators by banning masks in school. They’re setting a dangerous tone. For example, last week at a school board meeting in Tennessee, protesters threatened doctors and nurses who are testifying, making the case for masking children in schools. Intimidation and threats we’re seeing across the country are wrong. Today, I’m announcing a new step. If you work in a nursing home and serve people on Medicare or Medicaid, you will also be required to get vaccinated. More than 130,000 residents in nursing homes have had, sadly, over the period of this virus, passed away. At the same time. vaccination rates among nursing home staff significantly trail the rest of the country. I’m using the power of the federal government as a pair of health care costs to ensure or reduce those risks to our most vulnerable seniors. The threat of the Delta virus remains real. But we are prepared, we have the tools, we can do this, so all those of you who are unvaccinated, please get vaccinated for yourself and for your loved ones, for your neighborhood, for your community. And to the rest of America, this is no time to let our guard down.

President Biden has condemned states that are blocking mask rules in local schools, saying they are putting politics above public health. His administration has offered to step in and help the districts financially or cover board members’ salaries if the state imposes those sanctions.
On Wednesday, Education Secretary Miguel Cardona said that the administration would use the Department of Education’s civil rights enforcement authority to deter states from banning universal mask mandates in classrooms.
Hours after the Florida state board of education threatened to penalize the two districts, the Alachua school board unanimously extended its mask mandate for eight more weeks.
“That’s not defying me — that’s defying the state of Florida’s laws,” Mr. DeSantis told reporters in Broward on Wednesday. “That was the Legislature of Florida that said the parents are the ones that have ultimate responsibility for health, education and welfare.”
Vickie Cartwright, the interim superintendent of the Broward County Public Schools, said that district officials agreed with the governor’s view that children need to be in brick-and-mortar schools to do their best learning, and that was why the masks were necessary, amid so much virus spread.
“We want our students back in person,” Dr. Cartwright said in an interview on Wednesday. “We want to keep them there.”

Cuba’s health care system, long a source of national pride, is in acute distress, particularly in distant provinces.
After fending off the coronavirus last year, Cuba has been ravaged this summer by the highly contagious Delta variant, which has sent case rates soaring and swamped the country’s medical system.
More than 8,600 new cases were reported on Tuesday, about six times as many as the number of new cases just two months ago, according to Ministry of Health figures.
Oxygen supplies for Covid-19 patients are running low, and the factory that produces the nation’s canisters is currently shut down.
Mortuaries and crematories have been overwhelmed. The city of Guantánamo, for example, is dealing with a surge of deaths that on some days climbs to about eight times the usual number, a government official said. Cubans are posting heart-wrenching videos of dead relatives, saying that their loved ones died for lack of medical care.
This past weekend, after Cuba’s prime minister, Manuel Marrero Cruz, said that Cubans were complaining more about doctors and their poor service than they were about the shortages, nearly two dozen young physicians and medical students took to social media to state, one by one: “I am publicly declaring that doctors are not to blame for the collapse of the public health system.”
The move was a daring step in Cuba, where any public show of discontent may result in the loss of employment or even prison.
Cuba’s president, Miguel Díaz-Canel Bermúdez, acknowledged recently that the pandemic had “exceeded the capacity” of the Cuban health care system, but he blamed the U.S. trade embargo for the shortages the country suffers.
While the pandemic has strained medical systems around the world, the calamity in Cuba is particularly significant because the government has for decades held its free health care system up as a signal accomplishment of the socialist revolution. But the growing crisis has revealed a frayed system that, while often producing medical breakthroughs, is also denounced as ill-equipped and underfunded.
The Cuban Ministry of Health did not respond to several requests for comment.
Alexander J. Figueredo Izaguirre, a doctor in the Cuban province of Granma, said he was fired this year after he criticized the poor state of the country’s hospitals following the death of his grandfather.
“The funeral homes can’t cope, the hospitals can’t cope, the clinics can’t cope,” he said. “We have been struggling for a year and a half in this battle against this disease — without weapons — when hundreds and thousands of people are dying.”

World Health Organization officials warned on Wednesday that the Taliban takeover of Afghanistan was impeding efforts to address the coronavirus pandemic and other dire health crises there.
Gauging the spread of the coronavirus in Afghanistan has always been difficult because of a lack of testing. The average daily number of reported new cases peaked in late June at more than 2,000 and has since fallen sharply, according to the Our World in Data project at the University of Oxford. But it is likely that the figures do not reflect the actual spread of the virus.
Afghanistan’s vaccination efforts have struggled since they began in the spring, harassed by corruption, limited public health resources and widespread public skepticism. According to Our World in Data, less than 2 percent of Afghanistan’s population has been vaccinated.
“In the midst of a pandemic, we’re extremely concerned by the large displacement of people and increasing cases of diarrhea, malnutrition, high blood pressure, probable cases of Covid-19 and reproductive health complications,” Dr. Tedros Adhanom Ghebreyesus, the W.H.O.’s director general, said at a news conference.
He said that agency staff members were still in Afghanistan and were “committed to delivering health services to the most vulnerable.”
Many Afghans are vulnerable to diseases like polio, which has been eradicated in most of the world but is still endemic there. Fourteen million Afghans are suffering from hunger, United Nations officials said on Wednesday.
Aid groups are struggling to provide humanitarian assistance inside Afghanistan and to the tens of thousands of refugees a week who are fleeing to neighboring countries. Refugee camps, with their crowded and often unsanitary conditions, can become incubators for the virus, though many camps have fared better than experts initially feared they would.
U.N. officials said that their agencies in Afghanistan were in contact with the Taliban in an effort to coordinate aid and immunizations. Caroline Van Buren, a representative of the U.N. High Commissioner for Refugees, said that the Taliban had so far provided protection for all of the refugee agency’s offices in the country.
At the same time, though, the Taliban have resumed some of the practices common when they held power 20 years ago. Ms. Van Buren said that officials had received reports of women being prohibited from going to work, and, in some areas, barred from leaving their homes without being accompanied by a close male relative.

There wasn’t a single I.C.U. bed available in Alabama on Wednesday, a possible sign of what other states may confront soon amid a deadly surge of new infections in parts of the United States with low vaccination rates.
I.C.U. beds, where hospitals’ critically ill patients are treated, are filling up across Southern states, and Alabama is one of the first to run out. The Alabama Hospital Association said on Wednesday night that there were “negative 29” I.C.U. beds available in the state, meaning there were more than two dozen people being forced to wait in emergency rooms for an open I.C.U. bed.
The situation has grown desperate in Alabama, one of several states reporting a wave of cases driven by the highly contagious Delta variant and low vaccination rates.
In the week ending Aug. 12, one in five American I.C.U.s had reached or exceeded 95 percent of beds full. The crisis is concentrated in the South, with small pockets of high occupancy elsewhere in the country. The national average I.C.U. occupancy in 2010 was 67 percent, according to the Society of Critical Care Medicine, though the occupancy baseline changes depending on the place, time of year and size of hospital.
During other surges across the country, hospitals have been forced to improvise, expanding capacity by creating new I.C.U.s in areas normally used for other purposes, like cardiac or neurological care, and even hallways or spare rooms. Experts say maintaining existing standards of care for the sickest patients may be difficult or impossible at hospitals with more than 95 percent I.C.U. occupancy.
Alabama has never before faced this sort of I.C.U. crisis during the pandemic, the state health officer, Dr. Scott Harris, said on Wednesday in a television interview with WSFA12 News. Such patients are still being treated elsewhere in hospitals, including in “perhaps a regular room on a floor that’s been converted into an I.C.U.,” he said.
But the strain on hospitals threatens to overwhelm staff already stretched thin and endanger the quality of care for non-Covid patients, he said.
“In most parts of the state, the average person who has a heart attack today or is involved in a serious automobile accident, it’s going to be difficult,” Dr. Harris said. “The hospitals are going to have to be real creative in finding a place to be able to care for that patient.”
Last week, at least two hospitals in Houston were so overwhelmed with virus patients that officials erected overflow tents outside. Elsewhere in Texas, in Austin, hospitals were nearly out of beds in their intensive care units. And in San Antonio, cases reached levels not seen in months, with children as young as 2 months old tethered to supplemental oxygen.
Arkansas hospitals were also close to capacity.
Only 47 percent of people in Alabama are at least partially vaccinated, far lower than the national rate of 60 percent, according to a New York Times database.
On Monday, the seven-day hospitalization average hit 2,603, up from a low of 252 on June 26. Only January’s numbers were higher, when the seven-day average peaked at more than 3,300 on Jan. 10.
Gov. Kay Ivey of Alabama said last month that the surge in new cases was attributable to the large number of people who remain unvaccinated. On Friday, she reinstated Alabama’s state of emergency, which had expired in early July, in an effort to expand hospital capacity.
Dan Levin contributed reporting.

Paralympic officials in Tokyo on Thursday reported the first confirmed coronavirus case in the Olympic Village, five days before the Games are set to open.
The Olympic Village case is one of 16 total associated with the Paralympics so far.
The early Paralympic cases come as both Japan and Tokyo, the capital, are reporting record daily new cases. On Tuesday, the Japanese government extended the state of emergency in Tokyo and other regions until Sept. 12, a week after the end of the Paralympic Games. It also declared an emergency in seven more prefectures.
During the Olympic Games, which lasted from July 23 to Aug. 8, organizers recorded more than 500 cases within the so-called Olympic bubble. Only three of those people were admitted to the hospital, and no severe cases arose among those directly connected to the Olympics. Visitors from overseas were asked to travel only between their hotels and competition venues for their first 14 days in Japan, and athletes and others were tested daily. Those who tested positive were put into isolation and some athletes were even sidelined after a positive test. Paralympic athletes are expected to be under similar restrictions.
Just as with the Olympics, the Paralympics will allow almost no spectators, although the Tokyo organizers have said that they hope to admit limited numbers of students to some events. At a news conference this week, Seiko Hashimoto, president of the Tokyo organizing committee, said that organizers were implementing “watertight measures” to avoid large outbreaks.
Source: https://www.nytimes.com/live/2021/08/19/world/covid-delta-variant-vaccine/